Why does tracking your child's behavior change everything?
Doctors, therapists, and IEP teams work from data. When you show up with documented patterns, you're not asking anyone to believe you — you're showing them evidence. That's a completely different conversation.
"He's been having more meltdowns lately" doesn't move the needle. "He had four meltdowns last week — all between 3 and 5pm, all triggered by transitions, and redirection worked three out of four times" does. The difference isn't what you noticed. It's what you can prove.
Think about the last appointment you left wishing you'd said something differently. You were trying to remember what happened two weeks ago, in the middle of a hard moment, while managing the waiting room and whatever mood your child was in that day. That's not a memory failure. That's an impossible ask. Written documentation doesn't make you more credible — it gives your provider something concrete to work with in the 20 minutes they have.
Families in our community who started bringing the tracker consistently say the same thing: the conversation changes. Providers engage differently when there's something on the table besides memory. Testing gets ordered. Medication timing gets adjusted. IEP goals get written to reflect what's actually happening at home. It's the same information — just documented instead of recalled.
This tracker was built by caregivers for caregivers
It takes 30 seconds a day because that's all most parents have. It's not a clinical instrument. It's not an ABA data sheet. It's a parent advocacy tool — built to turn what you already notice into something professionals can actually work with.

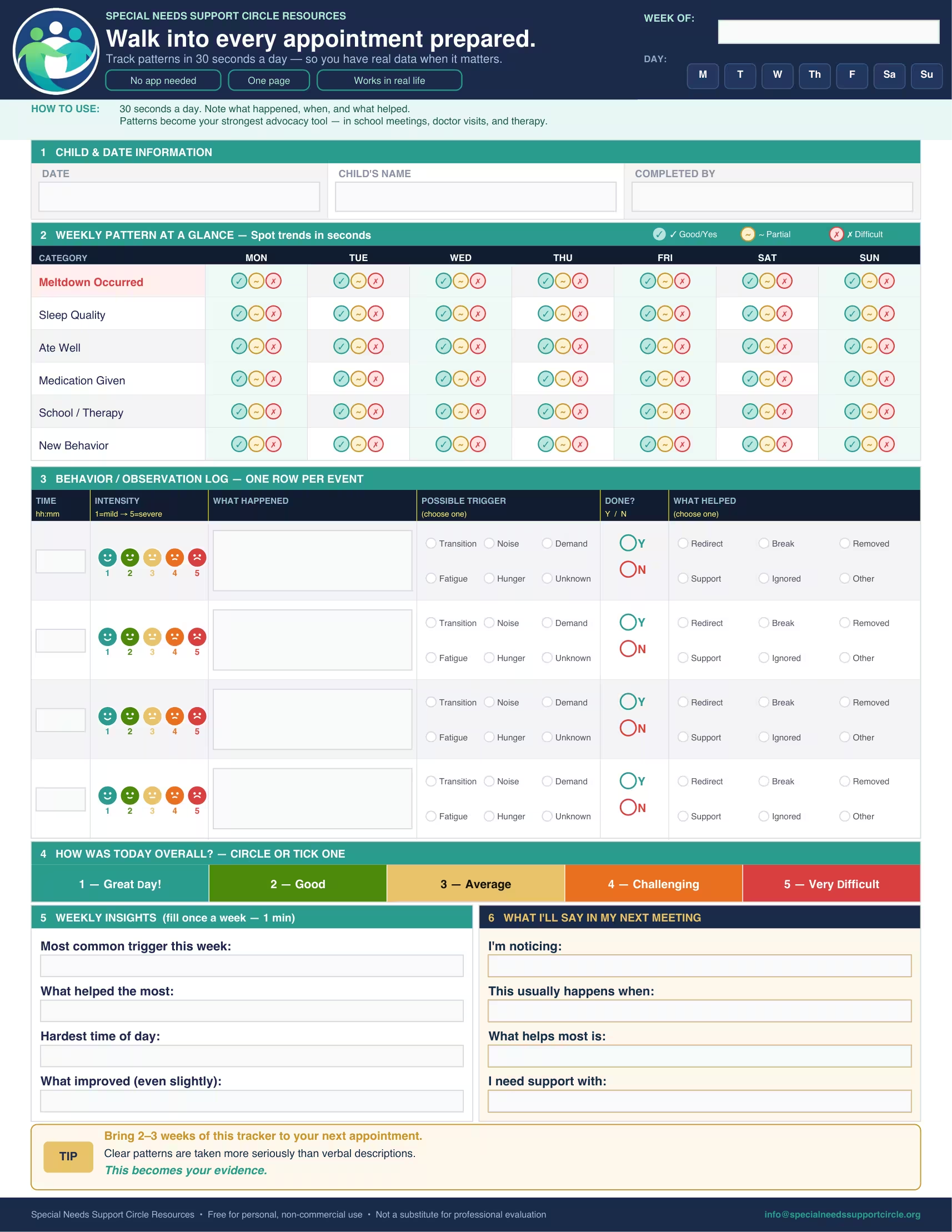
What does the Daily Behavior Tracker include?
One page per week. Every section has a job — and together they build the kind of picture that takes 10 minutes to explain at an appointment, or 10 seconds to show.
Weekly pattern grid
Check good, partial, or difficult each day for meltdowns, sleep, meals, medication, school or therapy, and new behaviors. Spot trends at a glance without reading through paragraphs of notes.
Behavior observation log
One row per event: time, intensity (1–5), what happened, the trigger category, and what helped. Fast to fill in the moment, useful for months afterward.
Daily overall rating
One number, 1 (great day) to 5 (very difficult). Not a clinical scale — a quick pulse on the week that shows providers whether things are trending up, down, or staying flat.
Weekly insights section
Most common trigger, what helped most, hardest time of day, and what improved — even slightly. Filled in once a week. Designed to show progress alongside problems.
"What I'll say in my next meeting"
Pre-written sentence starters that turn your tracker data into actual talking points — for IEP meetings, doctor visits, and therapy sessions. This section is the bridge between documenting and advocating. No other behavior tracking tool has it.
The fillable PDF works on any device — phone, tablet, laptop. The print version is optimized for paper — all form fields are replaced with blank lines. Both sent to your email when you sign up above.
How do you use the behavior tracker effectively?
Three steps. Total time: about 30 seconds for the daily check-in, one minute for the weekly summary. That's it.
Fill in the weekly pattern grid each evening
Just check good, partial, or difficult for each category. Don't overthink it — your gut impression is data. If you can't remember clearly, leave it blank. An honest partial record is more useful than a guessed complete one.
Log specific events as they happen — or right after
One row per event. Note the time, rate the intensity (1–5), write what happened, what triggered it, and what helped. You don't need paragraphs. "3:15pm / 4 / meltdown at transition / school pickup / deep pressure worked" is a complete record.
Fill in the weekly insights section — then use the meeting prompts
Sunday evening, five questions, one minute. What was the most common trigger? What helped most? What was the hardest time of day? What improved — even slightly?
Before your next appointment, read the "What I'll say" prompts. They turn your tracker data into sentences — specific, professional, hard to dismiss. The kind of sentences that make a provider stop typing and actually look at what you brought.

Haven't downloaded it yet? Both versions — fillable PDF and print version — sent to your inbox in seconds. Free.
How does behavior tracking help at IEP meetings, appointments, and therapy?
You're not tracking for the sake of tracking. Every row you fill in is preparation for a conversation you need to go differently. Here's what changes when you show up with the data.
Turn "I'm worried about" into "I've documented that"
Developmental pediatricians, psychiatrists, and neurologists see your child for 20–40 minutes. In that window, they're working from what you tell them. A tracker gives them three weeks of daily patterns to look at instead of relying on what you can recall under pressure.
"I'm noticing a pattern" is a different statement than "things have been hard." The first invites clinical curiosity. The second invites reassurance. Which conversation do you want to have?
Guide: How to document behavior for appointments →
Schools respond to documented data. Not general concerns.
If you're requesting a Behavior Intervention Plan (BIP), the IEP team needs baseline data — and parent-documented patterns are a legitimate source. The trigger categories in this tracker map directly to Functional Behavior Assessment (FBA) language, so you're already speaking the same vocabulary the school team uses.
If the school says your child's behavior "isn't a problem at school," your home documentation becomes the other side of the picture — the part they can't see and can't dismiss if it's written down.
Guide: Using tracker data as IEP evidence →
When you're in a hard week, everything feels like crisis. The tracker shows you what's actually changing.
There's something specific that happens when you document consistently: you stop carrying every hard moment in your head. It's on paper. You don't have to hold it anymore.
The weekly insights section asks what improved — even slightly. That question has a purpose. Hard weeks are real, but they can flatten your perception of what's actually trending. Seeing data across multiple weeks gives you something more accurate than exhaustion-filtered memory.
Caregiver support — reducing the documentation burden →

What behaviors should you track for your child's specific needs?
Every child is different. The tracker works across diagnoses — but the patterns worth watching, and the columns worth filling in most carefully, depend on what you're dealing with. Here's where to start based on your child's specific needs.
Which guide covers your specific situation?
The tracker gets you the data. These guides are what to do with it — in the specific situations where having that data actually changes the outcome.
Have questions about behavior tracking? Here are honest answers.
The questions parents ask when they've been dismissed too many times, or when they're about to walk into a hard appointment and wondering if the tracker will actually make a difference.
.png)